This December….
– 10 babies were enrolled in our program, including three orphaned newborns, one set of triplets, one baby with multiple congenital anomalies, one baby who was abandoned in a public space, one baby’s whose mother was not producing breast milk, and one baby whose mother was on chemotherapy.
– 7 women were enrolled including five with ruptured uteruses and subsequent hysterectomies, and two with severe infections following c-sections and subsequent.
– Nurses visited 138 women and babies
Baby Care Admission Story.
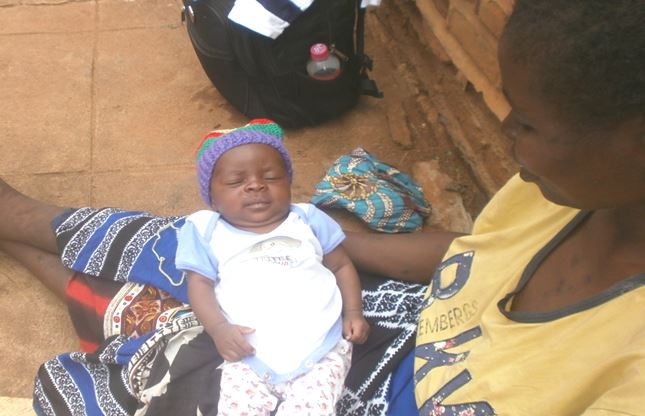
Mary was pregnant with her fifth child when she tested positive for HIV. She attended prenatal clinic and was able to receive anti-retrovirals to lower her viral load and decrease the risk of transmitted the disease to her baby. She went into labor a bit earlier than expected but delivered a healthy five and a half pound baby boy. Mary’s health seemed stable but she had developed a sore on her leg which, despite herself care, only seemed to get worse. The midwives who attended her delivery determined that the wound was severe enough to refer her to the regional hospital. There clinicians biopsied the wound and diagnosed her with cancer. Mary soon began chemotherapy but was forced to stop breastfeeding. At this point Mary and her baby boy were referred to Joyful Motherhood.
The World Health Organization recommends that HIV positive women exclusively breastfeed their babies to six months. WHO recommends anti-retrovirals during pregnancy and breastfeeding to decrease the risk of transmission. The risk of death from malnutrition or diarrheal illness for a young baby in Malawi outweighs the risk of HIV transmission from his mother. Formula is used as an absolute last resort, for babies who do not have access to the breast milk their need to sustain their lives.
Joyful Motherhood nurses are visiting Mary and her baby, providing formula, monitoring his health, growth and development and providing health education to Mary.
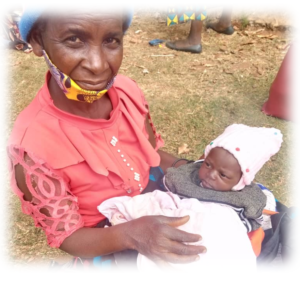
Mother Care Admission Story.
Sakina felt some early painful contractions on October 15th. She was a healthy 17 years old, expecting her first baby. Her mother accompanied her that day to the nearby health center to ensure that she labored under that watchful eyes of trained midwives. Soon after their arrival Sakina began seizing. She had developed eclampsia. Sakina was transferred to the district maternity hospital for high risk management.
Pre-eclampsia is a life-threatening disease of pregnancy. Even in 2019 our knowledge of pre-eclampsia is incompleted. We know risk factors but cannot predict who will be affected. When a woman suddenly develops high blood pressures and has protein in her urine she is diagnosed with pre-eclampsia. Delivery is the only cure. In the US a woman with pre-eclampsia is monitored carefully and delivered as soon as possible. In Malawi these early signs are often missed. There is often not much time between their onset and the quick acceleration of the disease. Pre-eclampsia may affect all the major organ systems and ultimately lead to death. Seizures indicate an advanced disease process (eclampsia).
On October 30th Sakina finally delivered a six pound baby boy. She was critically ill but clinicians believed she was well enough to go home and discharged her on November 4th. Sakina’s body was struggling to heal from the eclampsia and the c-section and she did not produce any breast milk. Her mother anxiously and loving tended Sakina and the baby, she saw them both struggling, but how could she leave Sakina to seek help for her grandson? She feared Sakina would deteriorate if left alone and where would she even go to get milk. Within one week Sakina’s baby boy wasted away and died. On November 11th Sakina’s mother could wait no more, she decided that to save Sakina, they would go to a mission hospital. She would have to pay for care but she would worry about that later. At the mission hospital doctors diagnosed Sakina with a severe infection and referred her to the region’s high risk maternity hospital. There Sakina was diagnosed with severe peritonitis and a necrotic uterus. On November 12th 17-year-old Sakina was taken to the operating room and underwent a total hysterectomy. Weak and critically ill Sakina stayed in the hospital for over a week. On November 20th when it was noted that her condition was not improving, she returned to surgery. Her wound was reopened more purulent material was washed from her abdomen, four drains were placed. For the next month she stayed in the hospital, her wound slowly healing. On January 4th Sakina complained of leaking urine and a fistula was noted. She was referred to the fistula center where she was taught about dressing changes and discharged home on January 6th. She was still leaking urine but would have to wait until her body was strong and healthy enough to undergo the first repair surgery.
Joyful Motherhood nurses first met Sakina while at the high risk maternity hospital. They followed her after discharge and will continue to visit her, monitoring her health and offering emotional support to her family until she returns for her fistula surgery.